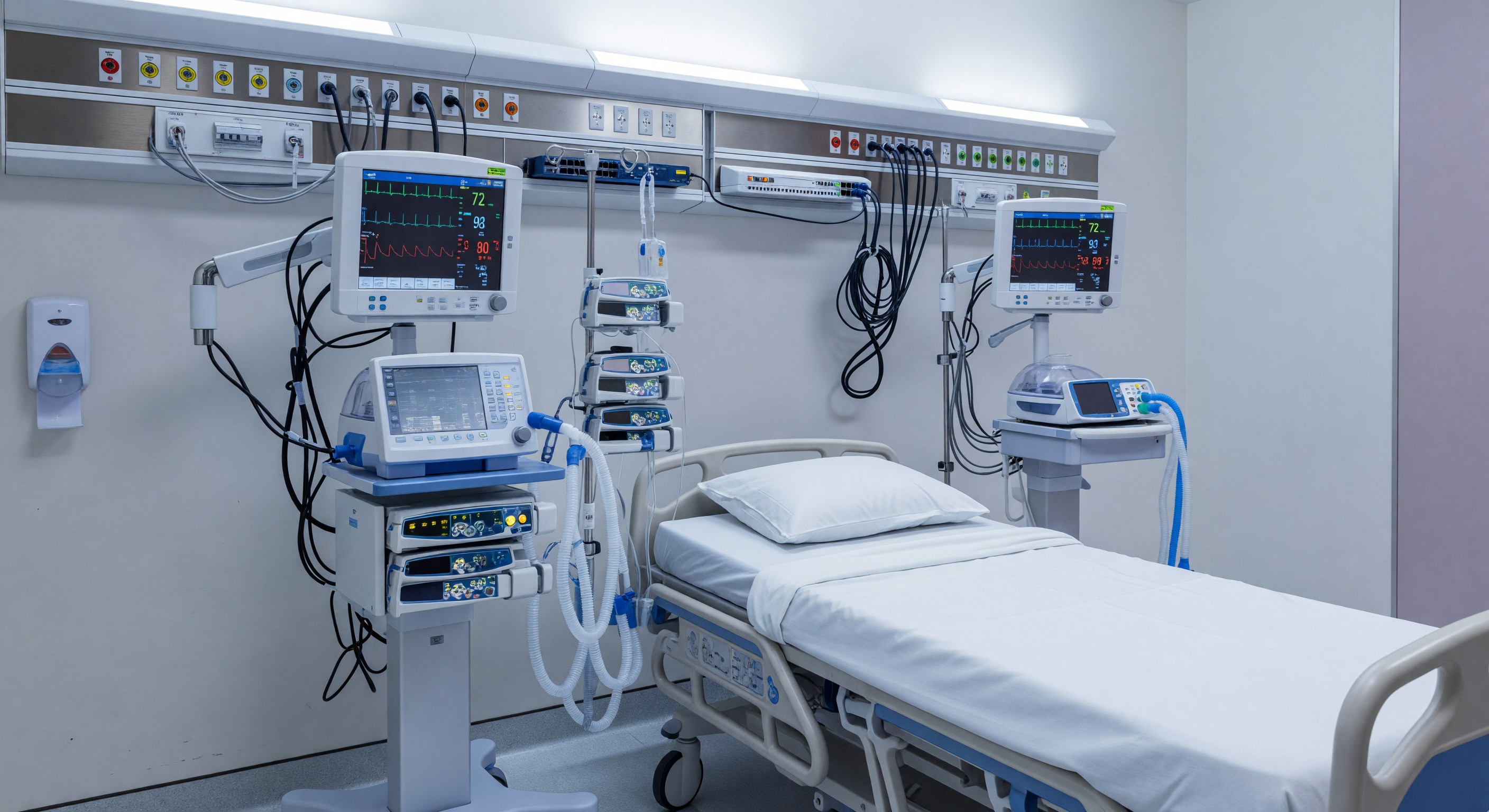
Patient monitoring systems—the physiological monitors, ventilators, infusion pumps, telemetry systems, and alarm platforms that continuously assess and manage patient condition—depend on facility infrastructure that facility directors must plan and maintain. Power reliability, network connectivity, mounting infrastructure, and physical space design all affect whether monitoring systems perform as clinically intended.
The interface between biomedical engineering, clinical informatics, and facility management defines the quality of patient monitoring infrastructure. When these functions work well together—planning power and network requirements during construction, coordinating maintenance schedules, and managing space changes that affect monitoring equipment placements—monitoring systems work reliably. When they don’t, clinical staff work around infrastructure failures with improvised solutions that introduce additional risk.
Power Infrastructure for Clinical Monitoring
Patient monitoring equipment requires reliable, clean power that meets the specific requirements of medical-grade electrical systems.
NFPA 99 Category 1 Power Requirements Patient care areas classified as Category 1 under NFPA 99—which includes intensive care units, cardiac care units, operating rooms, and emergency departments—must receive power from the Essential Electrical System’s Critical Branch. Monitoring equipment outlets in these areas must be connected to circuits served by emergency generators through automatic transfer switches that restore power within 10 seconds of utility failure.
Hospital-Grade Receptacles Patient care areas require hospital-grade receptacles—identifiable by the green dot and meeting NEMA standards for healthcare environments—that are designed for high-cycle use and provide more reliable contact than commercial-grade receptacles.
Isolated Ground Circuits Some sensitive monitoring equipment (particularly equipment used in cardiac procedures) benefits from isolated ground circuits that reduce electrical interference. Isolated ground receptacles are specified in new construction for critical monitoring areas when requested by clinical engineering.
Power Conditioning Highly sensitive monitoring equipment (polysomnography systems, certain research monitoring equipment) may require power conditioning—uninterruptible power supplies or power conditioners—that filter electrical noise and prevent power anomalies from affecting readings.
Outlet Density Planning Patient room and ICU bay outlet density planning must account for current and projected monitoring equipment. A critical care bay may require 12–20 duplex receptacles for monitors, ventilators, IV pumps, and support equipment, plus data outlets for network connectivity. Under-specifying outlet density in new construction creates the extension cord and power strip proliferation that creates both safety hazards and NFPA 99 compliance risks.
Network Infrastructure for Patient Monitoring
Modern patient monitoring systems are networked—transmitting continuous waveform data and alarm information to central monitoring stations, EHR systems, and clinical communication platforms.
Wired vs. Wireless Monitoring Bedside monitoring equipment may use either wired Ethernet connections or wireless connectivity:
Wired connections provide the most reliable, lowest-latency connectivity but require network outlet placement at each equipment location. New construction should include network outlets adjacent to each power outlet cluster at patient care positions.
Wireless telemetry allows monitoring of ambulatory patients without tethering. Telemetry systems require comprehensive wireless coverage throughout patient care areas, including typically poor-coverage areas like stairwells and transition corridors where patients are transported.
Equipment isolation: Patient monitoring networks should be isolated from general hospital IT networks through VLANs or physical segmentation, preventing clinical monitoring traffic from being affected by general network congestion or security events on the broader hospital network.
Network Bandwidth Planning Continuous physiological waveform transmission—ECG, arterial line, pulse oximetry—generates significant sustained bandwidth demands from multiple simultaneous patient connections. Network infrastructure planning for monitoring areas must account for the per-patient bandwidth requirement multiplied by the maximum patient census.
Alarm Routing Infrastructure Patient monitoring alarm routing—transmitting alarms to central stations, secondary alarm systems, and clinician communication devices—requires reliable network connectivity with priority traffic handling. Clinical alarm systems that share network infrastructure with general hospital traffic must have QoS policies that ensure alarm traffic receives priority delivery.
Mounting and Physical Infrastructure
Ceiling-Mounted Equipment ICU boom systems—articulated arms that position monitoring and support equipment above the patient bed—require ceiling structural support adequate for the combined weight of equipment and dynamic loading during clinical procedures. New construction should specify boom structural provisions at each critical care bed position.
Wall-Mounted Monitors and Displays Central monitoring station displays and secondary alarm displays throughout nursing units require structural blocking in walls for secure mounting. Retrofit mounting in existing walls may require opening walls to add blocking or using wall-mounted structural frames.
Pendant and Ceiling-Drop Cabling Power and data cabling for ceiling-suspended equipment (booms, ceiling-mounted monitors) must be routed through ceiling-drop assemblies that maintain code compliance while providing adequate cable routing capacity. These assemblies must be accessible for future cable additions as monitoring systems evolve.
Patient Room Layout Patient room layout should position monitoring equipment to allow unobstructed clinical access to the patient from the head of the bed while maintaining clear sightlines to monitoring displays from the doorway. Facility designers and clinical staff should collaborate on room layout to optimize both access and visibility.
Biomedical Engineering Coordination
The biomedical engineering (biomed) department manages clinical monitoring equipment at most hospitals—procurement, installation, calibration, and maintenance. Facility management and biomed must coordinate on:
Power and Network Planning Biomed specifies the power and network requirements for monitoring equipment; facilities implements the infrastructure. Early coordination ensures that infrastructure planning reflects current and projected equipment requirements.
Space and Renovation Coordination When patient rooms or monitoring areas are renovated, biomed must be involved to address equipment relocation, temporary monitoring arrangements during construction, and verification of power and network infrastructure before patient care resumes.
Maintenance Scheduling Some monitoring equipment maintenance requires coordination with facilities—electrical isolation for equipment adjacent to electrical work, network downtime windows for network-connected equipment updates, or ceiling access for above-ceiling cable work near monitoring equipment.
Equipment Lifecycle Planning Biomed maintains equipment replacement schedules; facilities needs advance notice of replacements that will require new power, network, or mounting infrastructure to avoid last-minute infrastructure projects.
Frequently Asked Questions
What’s the correct outlet circuit loading for patient care areas with intensive monitoring equipment? NFPA 99 requires that patient care area circuits serve a limited number of patient care areas to prevent overloading. In intensive care areas, circuits should be sized so that no single circuit serves more than a defined patient care area load. The specific circuit loading analysis should be performed by the electrical engineer of record during design, with clinical engineering input on equipment loads.
How should healthcare facilities handle power outages in patient monitoring areas? NFPA 99 requires that life-critical monitoring equipment in Category 1 areas be on Critical Branch power, which restores within 10 seconds from emergency generators. During the 10-second transition period, monitoring equipment with internal battery backup continues operating. Facilities should verify that all monitoring equipment in Category 1 areas is actually connected to Critical Branch circuits and that generator transfer tests confirm the 10-second restoration timeline.
Are there infection control requirements for patient monitoring equipment that affect facility design? Yes. Touch surfaces on monitoring equipment are frequently disinfected with healthcare-grade disinfectants. Monitoring equipment mounting and surrounding surfaces should be compatible with routine disinfection—no surface textures that harbor contamination, mounting hardware that allows cleaning of surrounding surfaces, and cable management that allows monitoring equipment to be cleaned without cable tangling.
What role should facility directors play when new patient monitoring technology is being evaluated? Facility directors should be involved in monitoring technology evaluation to assess infrastructure implications before purchase commitments are made. Key questions: Does the new system require power infrastructure changes? Network changes? New mounting hardware? Is the technology compatible with existing infrastructure, or does it require capital infrastructure investment alongside the equipment purchase? Identifying infrastructure requirements during evaluation prevents post-purchase surprises that delay deployment.