Pediatric and neonatal intensive care units face a security challenge unique in healthcare: the most vulnerable patients in the facility, cared for in units that attract intense family and visitor interest, in environments where the potential for abduction represents an existential reputational and regulatory risk. Healthcare security programs for pediatric and maternity settings require layered physical security that protects these patients without creating an environment hostile to the families who are essential to their care.
The Joint Commission’s environment of care standards and CMS conditions of participation both address infant security, and state health facility licensing standards in most states include specific provisions for infant unit security. Failure in this area has catastrophic consequences—infant abductions from healthcare facilities generate national media attention, immediate regulatory investigations, and lasting reputational damage.
The Infant Abduction Risk Profile
Hospital infant abductions are rare but devastating events. Research on infant abduction cases consistently identifies a profile of perpetrators and circumstances:
Perpetrator Profile Most hospital infant abductions are committed by women in the age range of their twenties to forties who may have experienced a pregnancy loss or desire for a child they cannot have naturally. These individuals often conduct pre-abduction reconnaissance—visiting the unit, asking questions about procedures, mapping access points.
Common Circumstances Abductions most often occur during periods of reduced observation—when nursing staff is attending to other patients, during shift changes, or when unit traffic is elevated and individual monitoring is harder. The abductor typically presents as a healthcare worker or authorized visitor to gain access to the infant.
Detection Methods Most attempted infant abductions are detected before the infant leaves the building because of electronic infant security tags that activate door alarms. The few successful abductions that have occurred typically involved technology failures, security response gaps, or units without comprehensive electronic security.
Electronic Infant Security Systems
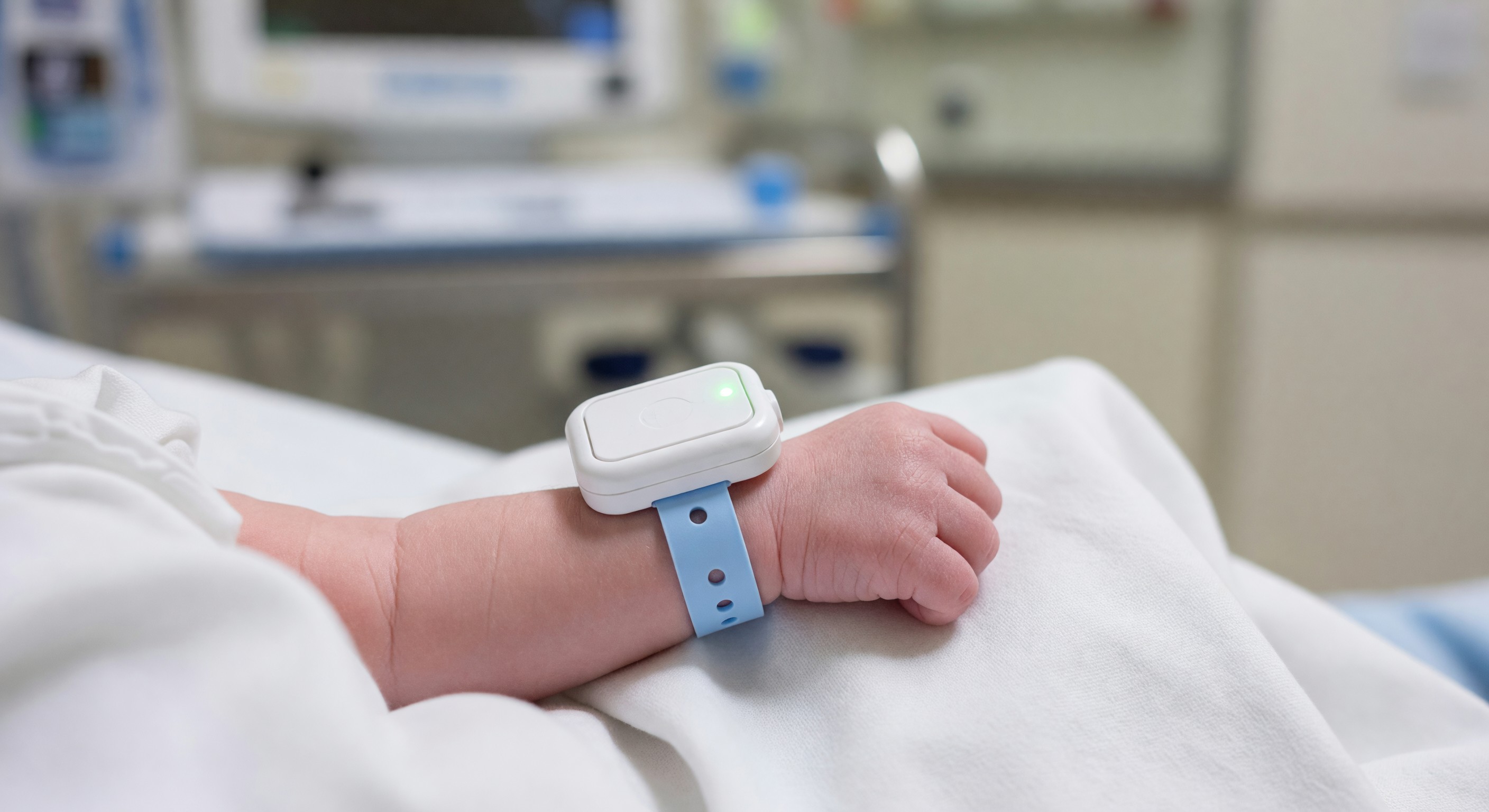
Electronic infant security systems (sometimes called infant security systems or ESIS) are the primary technology defense against infant abduction. These systems attach a transmitting tag to newborns and, in some implementations, to mothers, and monitor for:
Unauthorized Exit Tags generate an alarm when the tagged infant approaches exit doors or elevator entrances, triggering both a local alarm at the door and a centralized alert at the nursing station and security command center.
Tamper Detection Tags generate an alarm if removed or tampered with, alerting staff immediately if someone attempts to remove the security device.
Inactive Tag Detection Some systems can detect when a tag has not moved in an unusual period, potentially indicating that a tag has been removed and abandoned.
Mother-Infant Matching Advanced systems use matched tags for mother and infant that alarm if the matched pair is separated—helping prevent mix-ups during care as well as abduction attempts.
Leading infant security system vendors include Hugs (Rauland), Cuddles (Accruent), and CenTrak, all of which provide systems with varying levels of coverage, detection capability, and integration with access control and nurse call platforms.
Unit Access Control Design
Physical access control for pediatric and maternity units requires a layered design that balances security with family-centered care principles:
Primary Unit Entry The primary access point to the unit should have controlled access requiring either badge/credential presentation or intercom with visual verification and controlled door release. An airlock vestibule—two doors in sequence where only one can be open at a time—provides the most secure entry while allowing controlled visitor access. Staff with unit badges can enter directly; visitors are held in the vestibule while nursing staff verify their identity and relationship to a patient before releasing the inner door.
Visitor Management Integration Visitor access to pediatric and NICU units should be integrated with a visitor management system that tracks who has entered, the patient they are visiting, the time of entry and exit, and whether the visitor has received required education (hand hygiene, infant handling instruction for NICU). Visitor badges for pediatric units should be time-limited and include the specific patient name to prevent a single badge from being used to access multiple patients.
Secondary Exits All secondary exits from the unit—stairwell doors, service corridor connections, trash collection exits—must be alarmed and access-controlled to prevent unauthorized exit. These doors are often overlooked in security design but represent critical vulnerabilities in infant security coverage.
Elevator Security Elevators serving pediatric and maternity floors present a high-risk exit pathway. Elevator access restriction to authorized personnel during active infant security alerts, combined with floor-level intercept capability, is standard practice in comprehensive programs.
Visitor Management for Pediatric Settings
Pediatric and NICU visitor management requires balancing security against the established clinical evidence that family presence improves patient outcomes in these settings:
Designated Visitor Lists Parents should establish designated visitor lists at admission, specifying who is authorized to visit and—in custody dispute situations—who is specifically excluded. Healthcare staff must have processes for verifying visitor authorization against these lists before granting access.
Photo Identification Verification Pediatric and NICU units should require government-issued photo identification from all visitors, with identification documented and retained for each visit. This creates a record that supports investigation in the event of a security incident.
Visitor Restriction Protocols When clinical or security concerns indicate elevated risk—custody disputes, protective orders, suspicious behavior during prior visits—unit managers should have clear escalation paths for implementing enhanced visitor restrictions with security support.
Joint Commission Requirements
The Joint Commission’s environment of care standards don’t specify detailed technical requirements for infant security systems, but they do require that healthcare organizations identify and manage security risks to patients. Survey tracer methodology for infant security typically includes:
- Review of the facility’s infant security policies and procedures
- Physical inspection of unit access control measures
- Evaluation of infant security system coverage and alarm response procedures
- Review of documented drills or tests of infant abduction response procedures
- Assessment of visitor management practices
Many healthcare organizations conduct annual infant abduction drills that test the response of nursing, security, and administrative staff to a simulated abduction scenario. Documentation of these drills and the resulting improvement actions demonstrates proactive security program management.
Frequently Asked Questions
What’s the recommended response procedure when an infant security alarm activates? The response to an infant security alarm should be immediate, coordinated, and documented. Standard protocol typically includes: immediate lockdown of all unit exits (no one enters or exits), notification of security and hospital leadership, systematic search of the unit beginning at the alarm location, verification of all infants’ location and status, and notification of law enforcement if the infant is not immediately located. The entire response procedure should be documented and drillable.
How should hospitals handle situations where a custody dispute affects who can see a newborn? Hospitals should have a legal process for receiving and acting on court orders that restrict parental access to a newborn, coordinated through hospital legal counsel, social services, and security. In the absence of a court order, hospitals generally cannot legally prevent a biological parent from visiting, though security protocols can ensure that both parents are not simultaneously present if there are safety concerns. Social work involvement is essential in complex custody situations.
What’s the liability exposure if an infant is abducted from a hospital? Infant abduction generates liability exposure across multiple theories: negligent security (failure to implement reasonable security measures), negligent hiring or supervision of staff, and vicarious liability for staff whose negligence contributed to the abduction. Healthcare organizations that have comprehensive, documented, and consistently implemented security programs are in a significantly better legal position than those with inadequate or poorly maintained programs.
Do infant security systems also protect against infant mix-ups? Modern infant security systems with mother-infant matching capability can alert staff when a matched pair is separated—providing a technology check on infant identification in addition to abduction prevention. However, infant security systems are not a substitute for the comprehensive patient identification protocols (two-identifier verification before any care, medications, or procedures) required by Joint Commission standards.